Many procedures in veterinary medicine require anesthesia. In fact, this is more often true than it is in human medicine since our patients don't voluntarily hold still for any length of time. The main risk involved with most procedures that require anesthesia is the anesthesia, not the procedure we are performing. This is why you are asked to sign consent forms for any procedure that might require anesthesia.
Most anesthetic drugs depress the cardiovascular(heart) and respiratory(lung) systems. These drugs are detoxified and eliminated by a combination of the lungs, liver and kidneys. Although anesthetic risk cannot be totally eliminated, we can reduce it to a very low level. We do this in many ways:
Physical examination: All animals undergoing anesthesia at Village Veterinary Hospital receive a same day exam with special attention to organs and systems affected by anesthesia. This is true even if your pet was seen here the day before since we know that some problems can develop literally overnight. Other problems can come and go such as heart arrhythmias, escaping detection at one physical, but revealing themselves at the next.
Pre-anesthetic Blood Tests: We strongly recommend that all pets get blood tests before anesthesia. Senior pets 8 years and older are often required to get blood tests before anesthesia. Blood tests help us detect anesthetic (and surgery) risks that we could not find on the physical exam. To save you the inconvenience of an extra trip here, we have a laboratory in the hospital where we can perform these tests the same day as surgery. These tests include:
Kidney and liver tests - these organs must detoxify and eliminate many anesthetics
Tests for dehydration - this problem reduces circulation and increases risk of shock
Electrolytes - if these are abnormal, heart arrhythmias and cardiac arrest can result
Red blood cells - if these are low, oxygen delivery to vital organs can be compromised
White bloods cells - these are important for fighting infection
Platelets - these are needed for clotting(stopping bleeding) in traumatic procedures
Other diagnostic tests: If we find abnormalities on the physical exam or pre-anesthetic blood tests, your pet may need additional tests to determine the nature and severity of the problem. These may include urine analysis, electrocardiogram, radiographs(xrays), ultrasound or additional blood tests.
Intravenous catheter: We recommend these for all pets. This is a small tube that we can place in the vein before or during anesthesia. Anesthetic emergencies are rare, but when they occur, blood pressure is usually low which makes it difficult to find veins to deliver emergency drugs quickly. A catheter in the vein gives us a way to deliver emergency drugs quickly regardless of our ability to find the veins.
Doctor participation: It is legal in the state of California for a licensed veterinary technician to perform an entire anesthetic as long as a veterinarian is in the facility. In many hospitals, a veterinarian is never directly involved in anesthesia for xrays, dental cleaning or other procedures that do not require a veterinarian. However, at Village Veterinary Hospital, a doctor participates directly in every anesthesia. The doctor has six more years of scientific and medical education than a technician. We feel this enhances your pet's anesthetic safety.
Anesthetic drug protocols: Most anesthesias use an injectable drug to start anesthesia. In very short procedures, this may be all that is needed. In longer anesthetics we switch your pet to isoflourane gas anesthesia. This is widely considered the safest gas anesthetic in the veterinary profession. Because anesthetic can decrease heart rate, we also premedicate patients with an injection that counteracts this effect.
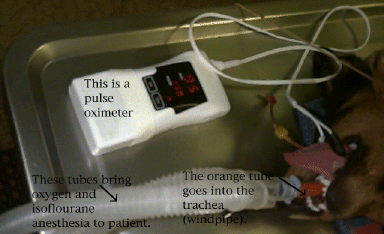
Monitoring: Most anesthetic emergencies start with respiratory arrest (the patient stops breathing). If they are caught at this stage, it is usually easy to reverse the situation with assisted breathing to maintain oxygen delivery. However, if this is not noticed, low oxygen levels will lead to cardiac arrest from which it is much more difficult to save the patient. Consequently, it is drilled into every doctor and employee to watch the breathing of pets under anesthesia very closely, even if they are not participating in the procedure and are just passing through the room. We also use a special respiratory monitor that sounds an alarm when a pet stops breathing. Heart rate and the depth of anesthesia are also monitored. While direct observation of the patient is at the foundation of anesthetic monitoring, we also use a pulse oximeter for many cases to supplement our observations. The pulse oximeter gives numerical measurments of heart rate and blood oxygen levels.
Thermal support: Anesthesia can also compromise a small, short haired, or ill pet's ability to maintain normal body temperature. Temperature monitoring and hot water bottles, heating pads and blankets are used as needed.
Individualized anesthetic protocols: Of course every patient's drug doses are adjusted for body weight, age or any other factor that affects anesthetic drug doses. The drugs used are modified as well in some cases. In addition, if we find problems in the pre-anesthetic evaluation, we take steps to reduce anesthetic risk associated with those problems. The most common precaution is fluid treatment of pets with dehydration, kidney or liver abnormalities. Fluid treatment involves injecting fluid either under the skin or in a vein. It is absorbed into the body and helps maintain blood pressure as well as helping the body to eliminate anesthetic drugs.
Delaying anesthesia: When serious problems are detected in the pre-anesthetic evaluation, the doctor may recommend delaying anesthesia until those problems are resolved. We know this can be an inconvenience for pet owners with busy schedules, but our first priority is your pet's well being.